
LGBT

With the start of a new year, I have been reflecting on how my personal history led me to my current work. I’ve always had an interest in workers’ rights; my grandfather was the last generation within our family to work in the Pennsylvania coal mines before moving on to a career in civil service. My grandmother, a factory worker, was an active union member. Growing up, family dinners included conversations about current events and politics, and stories of how generations before me were raised. These conversations instilled in me empathy, respect, and a belief that everyone deserves a fair chance to thrive.
To advance health equity and justice, we need to continue to support and expand progressive federal, state, and local policies that provide resources to help historically underserved communities—often communities of color—thrive.
My thinking on human rights, workers’ rights and health care policy were further influenced by formative texts like Barbara Ehrenreich’s Nickel and Dimed: On (Not) Getting By in America and Michael Moore’s documentary film, Sicko. My pursuit of a Master’s in Public Administration solidified my nonprofit and public health career and my commitment to initiatives that help families reach their full health potential.
The conditions in which we are born, grow, live, work, and age impact our health. Conditions such as economic stability, physical environment, education, food, and access to care all support or inhibit our health. In the public health community, these conditions are known as the social determinants of health (see figure below)1.
Let’s use childcare as an example for demonstrating the impact of social determinants. Think about the consequences of high cost or shortages in early childcare access:
This is just one example of how an issue not otherwise related to one person’s health, in this case childcare, cascades to impact health and overall well-being of a larger group.
Unfair and unjust policies, systems, and conditions in the U.S. have led to differences in health status based on race, gender, age, race, ethnicity or socioeconomic standing – especially among low-income communities and communities of color. For example:
In other words, white families who live in areas with increased household incomes will live longer than their low-income, Hispanic or Latino and Black or African American neighbors across the Bay.
To address these health disparities and inequities, many groups concerned about the well-being of individuals and communities are promoting social policies, practices, and systems-level change to achieve health equity. While there are many definitions for health equity, the one provided by the Robert Wood Johnson Foundation, a partner of Tides whose grantmaking is centered around health equity, states:
“Health equity means that everyone has a fair and just opportunity to be healthier. This requires removing obstacles to health such as poverty, discrimination, and their consequences, including powerlessness and lack of access to good jobs with fair pay, quality education and housing, safe environments, and health care.”
When we have successfully achieved health equity, everyone will have the opportunity to reach their full health potential without disadvantages stemming from social conditions.
Health inequities have many implications including economic costs, health care costs, quality of life, and duration of life. For example, more than 810,000 Americans die of heart disease or stroke every year. These diseases have fiscal repercussions, costing our healthcare system $190 billion per year and cause $126 billion in lost productivity on the job4. This is about more than just money, it’s about achieving social justice. In the words of Rev. Dr. Martin Luther King, Jr, “Of all the forms of inequality, injustice in health care is the most shocking and inhumane.”
To advance health equity and justice, we need to continue to support and expand progressive federal, state, and local policies that provide resources to help historically underserved communities—often communities of color—thrive. This means promoting and adopting policies to increase access, affordability and quality for education, child care, housing, economic revitalization, and more. California’s new Governor, Gavin Newsom, recently led by example in this area by appointing the state’s first ever surgeon general to urge policymakers at every level of government and leaders across the state to consider the social determinants of health, especially for children5.
In addition to policy advocacy and implementation, we also need to embrace compassion and empathy to develop a shared understanding that as a country, we must listen to one another, respect one another, and empower those most vulnerable.
In my current role, I leverage both my passion for health equity and collaboration to create policy change. Tides knows that complex social problems simply cannot be solved by a single funder or organization. This is especially true when it comes to achieving health equity. Health inequities are so deeply-rooted and so severe that it is going to take coordinated, multi-sector effort that bridges silos and inspire a shared vision to create lasting change. It’s exciting to be part of an organization that recognizes healthy individuals and communities are key to achieving a world of shared prosperity and social justice.
Of all the forms of inequality, injustice in health care is the most shocking and inhumane.
Rev. Dr. Martin Luther King Jr.
In partnership with the Robert Wood Johnson Foundation (RWJF), my time this year will be spent facilitating the ongoing alignment, collaboration, and integration of work across a group of nonprofits advancing policies at the local, state and federal level (such as Head Start, Supplemental Nutrition Assistance Program, Medicaid, etc.) to promote healthy, safe, and stable environments for all children and their families.
I’m excited to leverage Tides’ experience facilitating collaboration and commitment to advancing health equity to break down silos between stakeholders and sectors in support of positive impact. Tides’ work with RWJF is just one example of a long history supporting collaborations addressing health inequities.
Our partner Bay Area Regional Health Inequities Initiative (BARHII) is the coalition of the San Francisco Bay Area’s eleven public health departments committed to advancing health equity. BARHII recognizes that the health of communities transcends the jurisdictional county lines of its member health departments, and leverages the power of collaboration to drive policy and systems-level change. Their legislative policy platform includes areas that have not traditionally been within the scope of public health community policy priorities, including:
BARHII also developed a conceptual framework that illustrates the connection between social inequalities and health, and focuses attention on measures which have not characteristically been within the scope of public health department epidemiology. This framework6 has been used widely as a guide to health departments undertaking work to address health inequities:
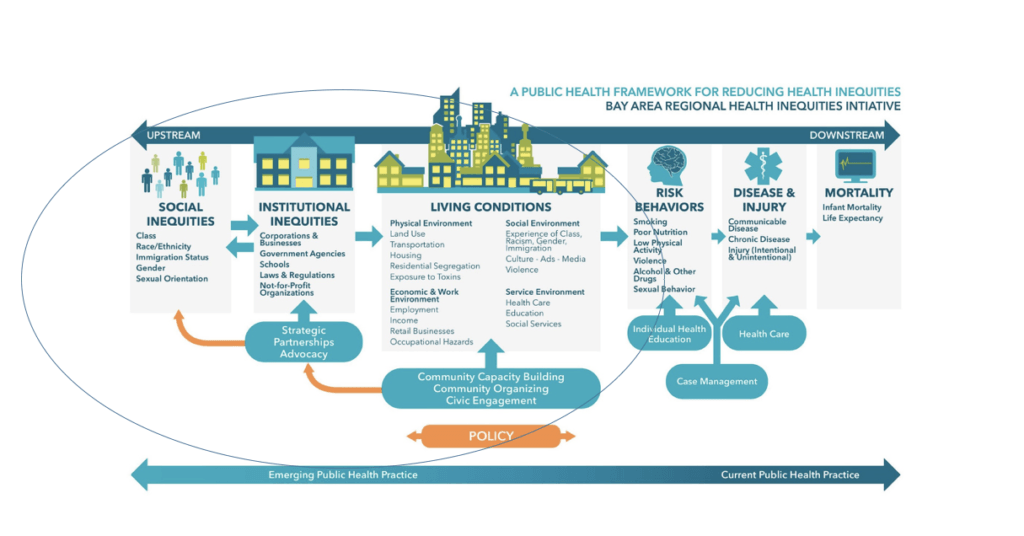
A Public Health Framework for Reducing Health Inequities from Bay Area Regional Health Inequities Initiative (BARHII)
Another Tides partner in the health equity space is the Center for Care Innovations (CCI). In an effort to reduce the risk of chronic disease later in life for all children to have healthy and vibrant futures, the Center for Care Innovations, in partnership with Genentech Charitable Giving, has launched the Resilient Beginnings Collaborative to improve the capacity of San Francisco Bay Area safety net providers to prevent, screen, and treat childhood adversity in pediatric care settings. Through a learning collaborative, seven participating safety net clinics are implementing tools to address trauma and promote resilience, with opportunities to learn from other clinics facing the same challenges through monthly webinars and in-person meetings. CCI itself was launched in 1999 through a collaborative grantmaking partnership between The California Endowment and Tides.
I am thrilled to be in a role that combines my passions for health equity and facilitating collaboration. The examples I outlined above – of coordinated, collaborative efforts working to advance health equity – remind me that we can achieve more together than we can individually. The reason health equity matters is simple: health is a basic human right.

LGBT

Corporate Partners

Philanthropy

Read the stories and hear the voices of social change leaders fighting for justice.